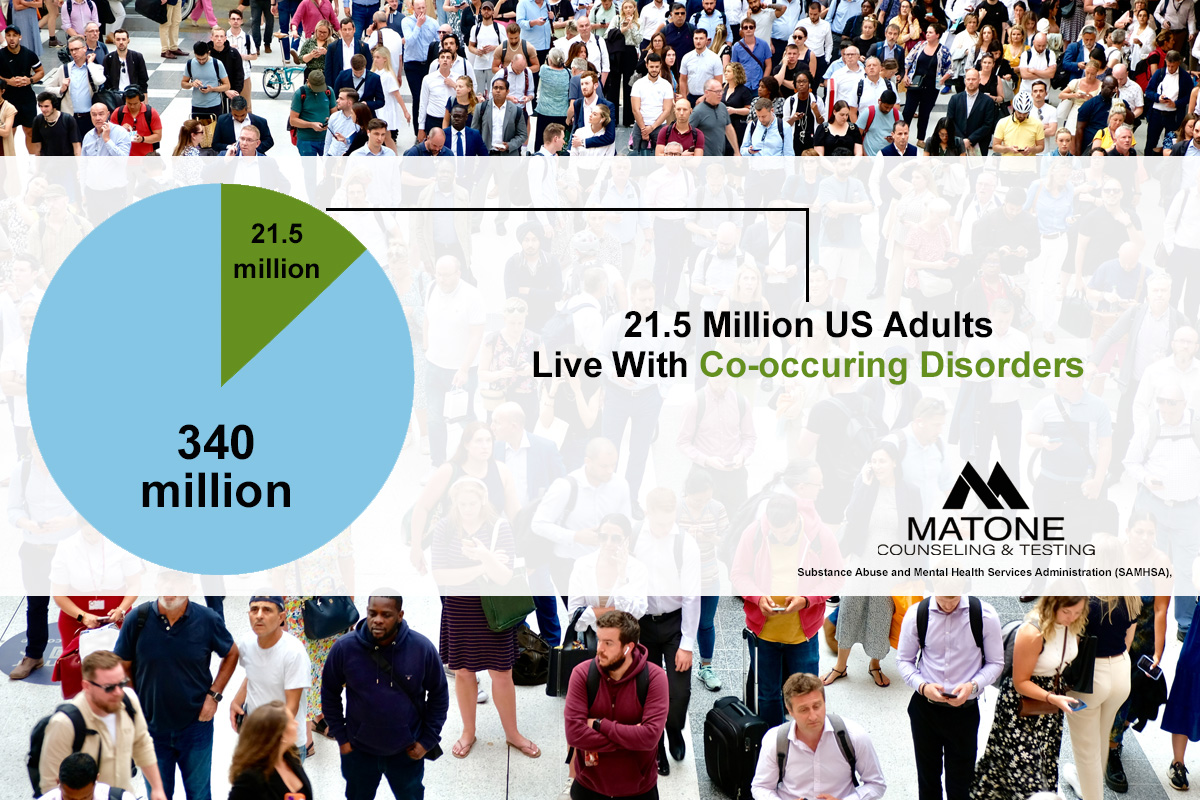
Dual diagnosis, also known as co-occurring disorders, refers to the presence of both a mental health condition and a substance use disorder (SUD) in the same individual. This complex interaction between mental illness and addiction is more common than many realize. According to the Substance Abuse and Mental Health Services Administration (SAMHSA), an estimated 21.5 million adults in the United States live with co-occurring disorders (SAMHSA, 2022).
In North Carolina alone, a 2021–2022 survey by SAMHSA reported that approximately 1.3 million individuals experienced both mental health challenges and substance misuse.
These statistics reflect the urgent need for comprehensive, integrated care that addresses the whole person rather than treating mental illness and addiction in isolation. Unfortunately, many individuals with dual diagnosis still face fragmented care systems that fail to meet their unique needs. They are often misdiagnosed, underdiagnosed, or left to navigate multiple service providers who may not communicate with one another. As a result, individuals struggling with co-occurring disorders can feel hopeless, isolated, or even ashamed.
Mental health conditions commonly associated with dual diagnosis include anxiety disorders, depression, bipolar disorder, schizophrenia, post-traumatic stress disorder (PTSD), attention-deficit/hyperactivity disorder (ADHD), and conduct disorder. There are many potential contributing factors to the development of co-occurring disorders, including genetic predisposition, early childhood trauma, environmental influences, and family dynamics. For example, someone who is genetically vulnerable to addiction and is prescribed Xanax for anxiety may quickly find themselves dependent on the medication, unintentionally setting the stage for long-term struggles.
Understanding the relationship between mental illness and substance use is critical in shaping effective treatment. In many cases, individuals turn to drugs or alcohol as a way of coping with emotional pain or unmanaged psychiatric symptoms. Conversely, chronic substance use may lead to the development or worsening of mental health conditions. This cyclical relationship creates a need for integrated treatment that acknowledges and addresses both sides of the equation.
Therapy specifically designed for dual diagnosis offers a compassionate and holistic approach to recovery. At the core of this approach is the bio-psycho-social model, which emphasizes the interconnectedness of biological, psychological, and social factors. Therapists working with co-occurring disorders recognize that healing must consider every layer of the client’s life. This model is person-centered, focusing on individualized treatment plans that reflect each client’s history, needs, and goals.
A significant barrier for many clients is fear—fear of being judged, labeled, or misunderstood. It’s important to understand that contemporary therapy does not view addiction as a moral failing but as a disease. Likewise, mental health struggles are not seen as personal weaknesses. Therapists strive to create a nonjudgmental, empathetic environment where clients feel safe enough to explore their experiences. Therapy becomes a place of healing, not harm.
The therapeutic relationship is essential to this process. Trust is built through consistency, compassion, and patience. Therapists at Matone Counseling & Testing meet clients where they are—whether that means working with someone in active use, in early recovery, or years into their sobriety journey. The focus is not on demanding immediate abstinence, but on fostering connection, insight, and gradual change. For many individuals, relapse is a part of the recovery process, not a failure. Therapy provides a safe space to reflect, recalibrate, and continue moving forward.
Medication management is often a component of treatment for dual diagnosis, especially when psychiatric symptoms require stabilization. Trust and open communication with providers are essential when navigating medications, especially given the risk of misuse or side effects. Some medications may serve multiple functions—helping both substance cravings and mood regulation, for example—but must be prescribed and monitored carefully. Being honest about substance use, even when it’s uncomfortable, is crucial to receiving the best possible care. While your medication prescriber will be in charge of the quantity and frequency of your medication, you can also talk to your therapist at Matone about what the experience of your medication is like so they can help you communicate those experiences to your doctor.
Therapists also help clients develop healthier coping strategies to replace substance use. This can include emotional regulation techniques, grounding exercises, communication skills, and self-care routines. There is no “one-size-fits-all” path to recovery. Some clients benefit from 12-step programs like Alcoholics Anonymous, while others connect more with SMART Recovery, and/or religious/spiritual communities. The goal is to support each individual in building a foundation that works for them.
Family involvement can also play a key role in the healing process. Addiction is often referred to as a “family disease” because its impact extends far beyond the individual. Therapy can involve family members in learning to set boundaries, repair broken relationships, and understand their own emotional reactions to a loved one’s struggles. Education and support for families can help them become allies in recovery, rather than unintentional barriers.
Evidence-based treatment modalities are widely used in dual diagnosis therapy and may include:
- Cognitive Behavioral Therapy (CBT): Helps clients identify negative thinking patterns, build awareness of triggers, and reshape behaviors.
- Dialectical Behavior Therapy (DBT): Teaches emotional regulation, distress tolerance, interpersonal effectiveness, and mindfulness.
- Acceptance and Commitment Therapy (ACT): Encourages acceptance of thoughts and feelings while committing to values-based action.
- Motivational Interviewing (MI): Enhances intrinsic motivation and helps resolve ambivalence about change.
- 12-Step Facilitation Therapy: Connects clients with peer-based recovery groups to foster ongoing support.
- Seeking Safety: A trauma-informed therapy focused on creating emotional safety and coping strategies for those with PTSD and SUD.
- Narrative Therapy: Allows clients to re-author their stories and view themselves beyond the scope of their illness.
- IFS-Informed Therapy (Internal Family Systems): Supports healing by exploring and integrating different “parts” of the self.
Integrated treatment is key to improving long-term outcomes for individuals with dual diagnosis. When mental health and addiction treatment are provided simultaneously by coordinated professionals, clients experience better care, reduced substance use, fewer hospitalizations, and an overall improved quality of life. This approach also reduces gaps in care, prevents duplication of services, and fosters long-term recovery.
Therapy, at its best, becomes a collaborative process. It is not about telling someone what to do—it is about working alongside them, helping them access their inner resources, and supporting them as they build the life they want. Healing happens in stages and in relationship. The client sets the pace. The therapist offers the map and walks beside them.
Recommendations for Clients Navigating Dual Diagnosis:
- Seek out a therapist or treatment center that specializes in dual diagnosis care.
- Ask if the program offers integrated treatment—meaning mental health and substance use services are addressed together.
- Be open and honest about your experiences. Your therapist is there to help, not judge.
- If possible, involve a trusted friend or family member for added support.
- Celebrate all progress, no matter how small. Harm reduction and self-awareness are important milestones.
- Connect with support groups or communities that understand the complexities of co-occurring disorders.
- Don’t be afraid to ask questions—about therapy, medications, or the recovery process.
- If you are in immediate danger or crisis, call or text 988 (Suicide and Crisis Lifeline).
Remember: You are not alone. Help is available, and recovery is possible.
Article by: Ari Barnaba

Ari Barnaba (she/her) is a graduate student studying Marriage and Family Therapy at Northcentral University. While she provides care to all clients, her training and focus is with couples and families on relational issues. Ari’s services are grounded in Bowenian Family Therapy and systemic theories. This means she facilitates clinical work to help clients balance personal autonomy and interactions with others. She guides clients to manage anxiety and move towards acceptance, healing, and growth. This also means that Ari sees anxiety, depression, and substance use issues as not just individual but relational concerns as well. She brings a non-judgmental and compassionate tone to her sessions, ensuring clients feel welcome and seen.
Ari has experience with adolescents and adults struggling with substance abuse, depression, anxiety, psychiatric disorders, and eating disorders. Working in substance abuse treatment for four years as a case manager, she ran multiple groups on coping skills, addiction, triggers, and recovery. She has a passion for utilizing evidence-based practices to support and help individuals, couples, and families. She believes in uniquely attending to each client’s needs.
References
Mueser, K. T., Noordsy, D. L., Drake, R. E., & Fox, L. (2003). “Integrated
Treatment for Dual Disorders: A Guide to Effective Practice.”
Drake, R. E., & Mueser, K. T. (2000). “Psychosocial Approaches to Dual
Diagnosis.” Schizophrenia Bulletin, 26(1), 105–118.
Substance Abuse and Mental Health Services Administration (SAMHSA). (2020).
“Treatment Improvement Protocol (TIP) Series 42: Substance Abuse Treatment
for Persons With Co-Occurring Disorders.”
https://www.samhsa.gov/mental-health/serious-mental-illness/co-occurring-disorders
https://link.springer.com/article/10.1007/s11469-022-00926-7